Since 2010, the School of Naturopathic Medicine at Bastyr University has paired first-year naturopathic students with core faculty mentors. This article explores the essence of the mentor/protégé relationship and gleans insights from students and faculty about the benefits of mentorship.
Abstract
Mentoring has existed since at least Ancient Greek times. The word mentor is thought to stem from the Greek word mentos, meaning “intent, purpose, spirit, passion.” Mentoring is a process for the informal transmission of knowledge and training support that the recipient perceives to be (typically) relevant to work, career, or professional development. Mentoring entails informal communication, usually face-to-face and during a sustained period of time, between a person who is perceived to have greater relevant knowledge, wisdom, or experience (the mentor) and a person who is perceived to have less (the protégé).
In 2010, a mentorship pilot program was created by the School of Naturopathic Medicine at Bastyr University, Kenmore, Washington, with the goal of establishing a mentoring relationship between first-year naturopathic students and knowledgeable core faculty members. The aim was to enhance each student’s ability to succeed throughout his/her medical education as well as invigorate the passion of the mentor for the field of naturopathic medicine. Intended to last throughout the student’s years of naturopathic medical school, the mentoring relationship was created to provide an ongoing human connection and role-modeling for the discussion and exploration of naturopathic medicine, guidance in career development including applications for residencies, and personal support. After the initial student evaluations of the pilot program were positive, the School of Naturopathic Medicine Mentorship Program was implemented in 2012.
In order to evaluate the program, an anonymous survey was conducted among participating students and faculty during the 2013-2014 school year. This survey provided important data to support the belief that ongoing personal faculty contact with first-year students provides for a more enriched educational experience and that students may be more likely to reach competency domains and benchmarks in areas such as professionalism. Faculty have also evaluated the program and remarked that teaching is especially rewarding when there is continuity in educating and modeling clinical skill development and professionalism to a cohort of students whom they have personally helped to develop through each stage of the student’s education.
Introduction
At graduation, a student receiving a doctorate in naturopathic medicine recites an oath before an attentive gathering of witnesses that includes these statements:
I will honor my teachers and … dedicate myself to supporting the growth and evolution of naturopathic medicine [and] I will impart knowledge of the advanced healing arts to dedicated colleagues and students.
This solemn pledge is readily fulfilled by faculty in a naturopathic medical school setting as faculty members dedicate their careers to the growth of the profession through the formal education of future naturopathic medicine students. However, what makes naturopathic medical students thrive in this environment goes beyond what is taught in the classroom and during clinic rotations. A student benefits most when careful attention is paid by attentive and nurturing faculty members who directly help refine each naturopathic medical student’s development. This happens through an age-old process called mentorship. Mentoring is very different from the traditional lecture-style educational format. Rather, mentoring is an intentional partnership through which someone shares knowledge, skills, information, and perspective to foster the personal and professional growth of someone else. Mentoring is about helping the students cultivate skills to become well-rounded physicians, each of whom will be unique. In this way, mentoring is very different from lecturing; the emphasis of mentoring is more about students and what they will discover even more than it is about what the mentor knows. Mentors strive to create the learning environment in which this discovery will occur for students.
This has significant implications for the naturopathic profession at large. Each member of the naturopathic medical profession has pledged to adhere to the principles of docere. Docere is a Latin word meaning “to show, teach, or point out.” The hope is that this directive would apply not only to naturopathic physicians’ patients but also to their colleagues and all other students of natural medicine.
The intent of this paper is to report on the mentorship program unique to the Bastyr University (BU) School of Naturopathic Medicine, Kenmore, Washington. The School of Naturopathic Medicine Mentorship Program (SNMMP) offers a model of how mentorship can be applied to help naturopathic medical students as they strive to learn from active members of the naturopathic profession. This could inspire the development of a simple preceptorship between a practicing naturopathic physician and student or perhaps the willingness to establish a small group mentorship program for naturopathic medical students in a successful, multipractitioner clinic setting. Beyond that, these relationships could develop into a formal or informal preceptorship or residency opportunities for naturopathic medical students, which would serve to promote the education of the members of our profession.
Bastyr University School of Naturopathic Medicine Mentorship Program
Faculty mentors were each paired with a small cohort of naturopathic students, providing support, guidance, and development of the multifactorial process of becoming a naturopathic physician. This relationship was designed to be an informal and nonevaluative relationship between each core faculty mentor being paired with the same small cohort of students throughout the students’ years of education and clinical training. Starting with the pilot stages of the program and further developed in the established mentorship program, it offered first-year and second-year students early exposure to fundamental clinical skills training through weekly meetings with their naturopathic faculty mentors to discuss actual case studies and topics related to becoming naturopathic physicians. This took place in a variety of formats, such as didactic case presentations, group and individual exercises, case-based problem-solving sessions, and visits from or to successful naturopathic physicians in the community. Further role-modeling was provided through clinical observation of these physician mentors early in the students’ training. In the latter part of the students’ education, faculty mentors continued to provide support and guidance, typically individual meetings with their cohort of protégés, on diverse topics (eg, future career development including the completion of residency applications, collection of letters of support, investigation into preceptorships).
Program Description
Understanding and meeting student expectations
At the beginning of each school quarter, students are encouraged to state their goals for and expectations of the program. Students are also asked if they have particular topics or interests in naturopathic medicine that they would like to explore during the mentorship program. They are encouraged to offer ongoing suggestions and requests on how the program may best supplement their educational experience. Mentors are aware of what is taught in the syllabi (eg, basic sciences, botanical medicine) and in some cases, meet with some of the professors to get handouts to help integrate cases that are more relevant to the students’ studies.
Mentorship format
Each faculty mentor has the freedom and flexibility in approach and format for mentorship meetings (eg, type of cases, format of presentation, readings, handouts). Faculty are also open to pursue other interests that students have or that they determine are important for students to know to become excellent physicians.
School of Naturopathic Medicine Mentorship Program curriculum
Each faculty mentor provides resources that are available via the web-based student portal Moodle (eg, handouts, outlines) within the 13 sections listed in Table 1. These sections serve as the outline for the topics to be covered by the end of 2 quarters. Each section has several pages of explanations and handouts. This is intended to provide a place for students to organize, record information, and read more about the topics that are covered in the group sessions.
General subjects
The primary topics covered in the mentorship program are divided into main sections with 3 different foci: being a naturopathic physician (1-11), being a naturopathic student (12-18), and the patient (19-24):
- Exploring what it means to be a naturopathic physician
- What are the qualities that one looks for in a physician?
- Professional and ethical behavior including respect, responsibility, competence, compassion, personal and professional integrity, honesty, and confidentiality
- Lifelong learning, how to stay current in the field
- Exploring options and making good choices, being open to all possibilities
- Enthusiasm can be contagious!
- Defining and choosing your career path
- How does one measure success?
- Yes, you can make a difference in this world
- The importance of maintaining balance in one’s life and paying attention to personal well-being
- The business, the practice, and the art of medicine
- Learning about and incorporating the philosophy and principles of naturopathic medicine into the student’s education, training, and future clinical practice
- Integrating the academic pursuit of knowledge with practical clinical training
- Clinical problem-solving skills and decision-making strategies
- Challenges along the way and strategies to meet those challenges
- Critically reflective and independent thinking
- Verbal, nonverbal, and written communication skills
- Interpersonal relationships
- Patient-centered medicine
- Giving your full attention to your patient and being present with your patient
- Being an encouraging and attentive listener: listening with sensitivity; practicing reflective listening
- Listening to your patients for content, beliefs, feelings, attitudes, and hidden meanings
- Caring for your patients and the practice of empathy
- Creating a safe and comfortable atmosphere for patients
Group Meetings
Each week starts with a few minutes of allowing the students to state how their classes are going and whether they have any questions, concerns, or follow-up on previous discussions. The group and individual meetings (see below) provide students with a reliable clinical faculty member with whom they can receive support and guidance in their clinical development throughout at least the first 2 years of school.
Case Studies
Because of unanimous feedback that students enjoyed working through actual patient case studies and “real world” situations, discussion topics are covered mainly through the context of actual case studies. These topics are chosen as they relate to topics being covered in basic science materials or to student interest. The cases serve as the stimulus and context for students to search out the information they need to understand the clinical presentation. Unlike the lecture-style classroom, which can sometimes create isolation, the case study activity encourages students to have a more “round-table” discussion; they are provided somewhat ambiguous details of a case and invited to “interview” faculty before making clinical summaries and linking clinical pearls.
Bringing in actual cases helps give students an appreciation of the complexity of case analysis and management of naturopathic medicine. They also best illustrate professional, ethical, and legal considerations such as dealing with cases of high-risk, noncompliant patients.
Case presentations are done in subjective objective assessment and plan (SOAP) format each week. Before presenting these SOAP notes, some mentors review naturopathic philosophy (including the teachings of John Bastyr, ND) and the components of taking a case. Emphasis is also placed on prioritization, which is based on such considerations as risk of morbidity and mortality, as well as the patient’s goals.
Verbal case presentation format
The rationale and expectation for verbal case presentations at Bastyr Center for Natural Health (BCNH), Seattle, are emphasized. Faculty explain that this format best engages one’s colleagues because it conveys the essentials of the patient’s condition to team members so that all can learn and participate during ongoing discussions of evaluation and management.
Role play
Participants also practice interviewing skills through role play. The students are asked to be the interviewer as the mentor plays the role of the supervisor or a standardized patient. First, the students are asked to share whatever questions come to their minds for the presenting symptom. Then their interview processes are reviewed, allowing them to practice organizing and defining their interview into a history of present illness.
Live patient interaction
Patients from BCNH were brought in to help facilitate learning in several ways. First, students are free to ask the patients about general topics such as how they came to see a naturopathic doctor, what the experience has been, or what information the patient thinks naturopaths in training should know. In these sessions, students asked questions like, “What do you think patients wished their doctors would know to help them follow their treatment plan?” and, “How do your naturopath and your conventional medical doctors interact?” The patients give students some feedback about the personal and social factors that may influence the patients’ response to therapy.
The goal of live patient interaction is to help students develop the art and skill of taking case histories and to enhance communication and professionalism. Students are also asked to volunteer to sit one-on-one with the patient to interact while the rest of the group observes. The students are given the opportunity to practice professionalism and to engage with empathy and respect. The mentor facilitates this interaction and gives feedback and instruction.
Some sessions are also spent on reviewing clinical pearls. For example, in one session, faculty related the following anecdote about Dr Bastyr that illustrates his entire philosophy: When Fernando Vega, MD, asked Dr Bastyr about which naturopathic modality he liked the most, Dr Bastyr answered, “Whatever works.” This story encourages students to keep an open mind about everything they are learning because it is best to utilize all of the modalities in the therapeutic toolbox.
Classes on therapeutics are incorporated into the mentorship program via class handouts and several copies of botanical medicine books. In one instance, the students were instructed to look over a list of herbs pertaining to the organ system that they were studying (adrenals), come up with a botanical formula, and state their rationale. Another time, the group practiced formulation skills, and 2 of the students who really applied themselves were awarded a bottle of the actual formulation.
Movie night
SNMMP incorporates media into the curriculum as well. At one of the group meetings, students watched excerpts from the movie The Doctor (1991), and a discussion was started about the doctor-patient relationship (in the movie, a surgeon learned empathy for the patient when he becomes a patient). Students are also given a list of other films that illustrate the patient-doctor relationship, including 50/50 (2011) and Awakenings (1990).
Individual meetings
Students are encouraged to seek assistance and guidance to make the adaptation to the responsibilities and stresses of naturopathic medical school more manageable. Seeking help in a timely manner keeps problems from becoming greater difficulties. These meetings for advice and mentorship are offered on an as-needed basis, whether during office hours or via email.
Protégé participation in clinic shifts
Students are given the opportunity to work with clinical faculty members whom they regularly shadow in the clinical setting. This helps model professional skills, including empathy, confidentiality, and communication. It also helps students develop an appreciation for the complexity of case analysis and management and lets them explore the psychosocial aspects of the patient experience. Students have the opportunity to observe how naturopathic principles and philosophy are incorporated into their education and future practice.
Coordinating peer mentorship and preceptorships
Advising and coordinating peer mentorships and preceptorships with practicing naturopaths can encourage, inspire, and teach students how to be best prepared for postgraduate plans like residencies, other training opportunities, or starting a practice.
For one session, a successful graduating student was invited to speak during group meetings on a variety of topics: how to study, how to prepare for clinic, how to maintain a healthy balance between medicine and personal life, and postgraduation plans. The protégés reported that they closely identified with some of the experiences that the graduating student shared and were encouraged by the graduate’s growth that resulted from the educational and training process at BU.
Method
A confidential questionnaire was distributed to students in the mentorship program through a web-based survey from Survey Monkey. The data were collected electronically for organization, analysis, and confidence purposes. This method was also used to preserve confidentiality and improve student and faculty participation.
Results and Discussion
Quantitative analysis: School of Natural Medicine Mentorship Program Student Survey, 2013-2014
First-year and second-year naturopathic medicine students were asked to rate their level of agreement with items regarding their overall satisfaction with SNMMP via a survey using a rating scale of 4 for “Completely Agree” to 1 for “Completely Disagree.” Fifty-eight students participated in this confidential survey of the 206 students who are in the first-year and second-year classes.
The highest-rated item for this category is, “I feel that I would benefit from some form of ongoing mentorship throughout my education and clinical training at BU,” with an average rating of 3.82 out of 4.0 (Figure 1). The lowest-rated item was “Shadowing a doctor on shift at BCNH has helped me to appreciate the practice of naturopathic medicine,” with an average rating of 3.41.
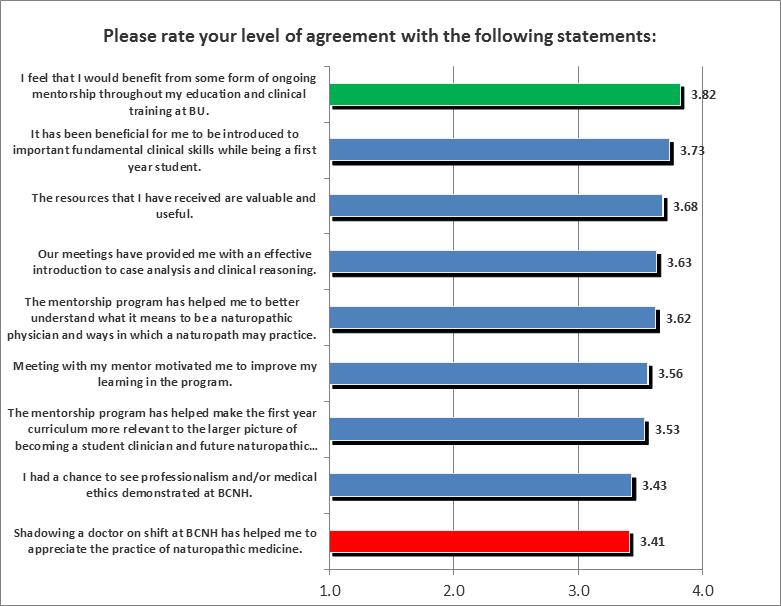
Figure 1. School of Natural Medicine Mentorship Program student survey responses.
Rating scale: 4 for “Completely Agree”; 3 for “Mostly Agree”; 2 for “Mostly Disagree”; and 1 for “Completely Disagree.”
Qualitative Analysis
The following is a categorized summary of students’ comments.
Survey Item: “What aspect of the mentorship program do you like the most so far? Why?"
Of the respondents, 92.5% praised the program, and 7.5% of the comments were constructive in nature; the comments that were constructive in nature stated scheduling conflicts as the primary area of concern.
Below are the specific reasons students stated for liking the program (some respondents named more than one criterion). In all,
- 32.5% of respondents stated they benefited from the mentorship experience itself.
- 30% of respondents stated they felt this program led to learning more clinical skills and prepared them in how to be physicians.
- 17.5% stated that they appreciated learning in a small-group setting.
- 12.5% of respondents stated that they appreciated the cases and content provided during the meetings.
- 5% stated that they appreciated getting one-on-one attention.
Survey Item: “What are your three suggestions for improving the mentorship program?”
More than one-third (35.8%) of the respondents offered suggestions. They stated that the main area that needed improvement is scheduling conflicts. The most useful comments included requests for “more variation in mentors’ availability/meeting time” and for organizers to “Publish the time of the meeting ahead of the quarter so we can organize our schedule better.” In all,
- 20.7% of the respondents had various suggestions for their mentor such as “More time for individual attention” and “Seeing our mentors ‘in action.’"
- 11.3% suggested having more field trips.
- 5.7% of the respondents requested that the groups remain small in number.
- 5.6% suggested giving a better introduction of the program at the beginning of the school year.
- 3.7% made suggestions on the content.
Survey Item: “Additional comments and/or experiences you would like to share”
In all, 68.4% of the respondents praised the program, and 31.6% of the respondents had comments that were constructive in nature.
Quantitative Analysis: School of Natural Medicine Mentorship Program Faculty Survey, 2013-2014
Core faculty at BU were asked to rate their level of agreement with items regarding their overall satisfaction with SNMMP using a rating scale of 4 for “Completely Agree” to 1 for “Completely Disagree.” All faculty mentors (except the director) participated in this confidential survey (Table 2).
Rating scale: 5 for “Strongly Agree”; 4 for “Agree”; 3 for “Somewhat Agree”; 2 for “Disagree”; and 1 for “Strongly Disagree.”
Conclusion
The goal of SNMMP has been to provide support and guidance in developing fundamental clinical skills, increase clinical experience and understanding, provide a role model within clinical faculty, and integrate naturopathic philosophy and principles into case analysis and professionalism through patient-centered learning. The desired outcome was to increase student satisfaction in their educational experience, and the student and faculty surveys indicated benefit in this area. Supported by results of the surveys, the mentorship relationship among students and faculty at BU School of Naturopathic Medicine fosters and guides career growth, develops skillsets, and gives students the extra inspiration they need to launch successful careers in natural medicine.
May each member of the naturopathic medicine community practice docere in the most comprehensive sense of the word, including reaching out to naturopathic colleagues and students with mentorship opportunities for the promotion, growth, and strength of our profession.
Acknowledgment
The authors of this paper, who developed and participated in the program, would like to heartily thank the Bastyr University core faculty mentors who also participated in and contributed to the development of the Bastyr School of Natural Medicine Mentorship program: Sarah Acosta, ND; Laurie Cullen, ND; Christian Dodge, ND; Katherine Raymer, ND; Jamey Wallace, ND; and Eric Yarnell, ND. Thank you, mentors, for enriching the education of the future generation of naturopathic physicians by your dedication to mentoring individual students.










